Is Keratoconus Rare? Prevalence, Risks & Early Diagnosis
If you’ve come across the word “keratoconus,” you might be wondering just how common (or uncommon) this condition really is. Maybe a doctor mentioned it, or someone you know has it.
Medically Reviewed By:
Dr Advaith Sai Alampur
Leading LASIK & Refractive Surgery Expert
Condition:
Treatment:
In this article
- LASIK reshapes the cornea to correct nearsightedness, farsightedness, and astigmatism.
- The procedure is FDA-approved, safe, and uses modern laser technology for precision.
- Candidates should be over 18, have a stable prescription, and healthy corneas.
- Short-term side effects can include dry eyes, halos, glare, or temporary vision fluctuations.
- Most patients achieve stable, long-term vision improvement and are satisfied with results.
- LASIK doesn’t stop natural age-related changes, so reading glasses may still be needed later.
Whatever brought you here, you likely have questions. Is keratoconus considered rare? Who gets it? What does that mean for you or your loved ones?
Let’s unravel the mystery together in a simple, no-nonsense way. By the end of this, you’ll have a much clearer picture of where keratoconus fits in the world of eye conditions.
What Is Keratoconus Again?
Before we jump into how common it is, let’s do a quick refresher.
Keratoconus is a condition where the cornea, the clear, dome-shaped front part of your eye, becomes thinner and starts to bulge outwards into a cone shape. This irregularity messes with how light enters the eye, making vision blurry or distorted.
It can’t be fully corrected with regular glasses, which is why many people turn to specialized treatments like custom contact lenses or corneal cross-linking.
Now, onto the big question…




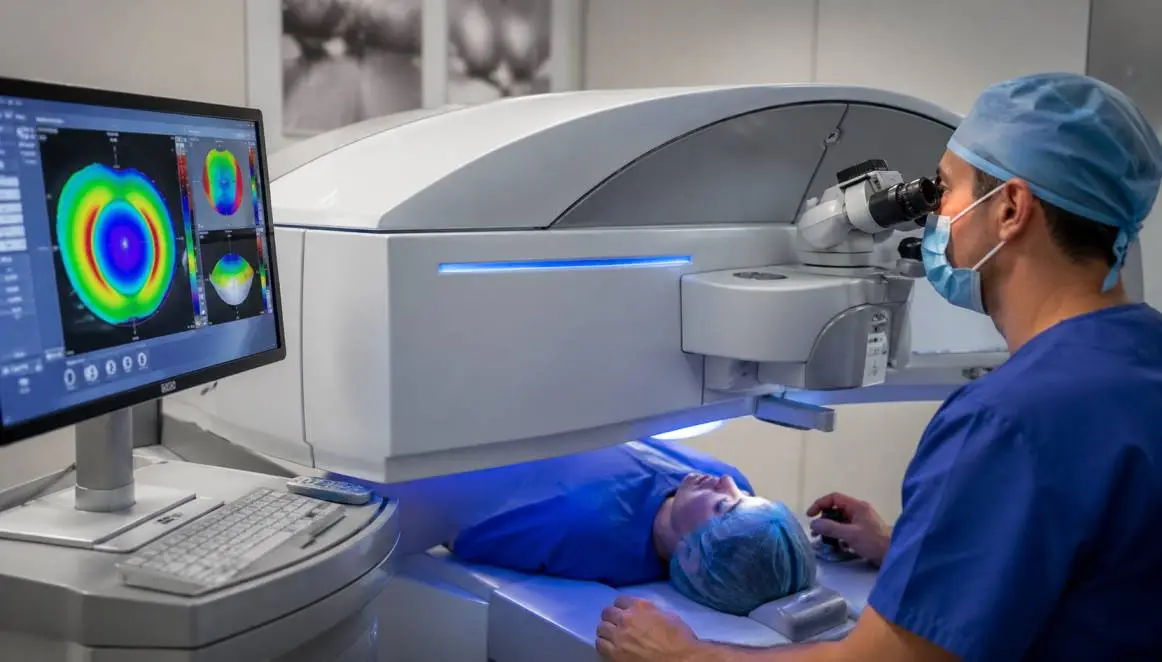
(Put Real times images and shorts of Dr Avdaith Sai Consulting, Operating on Patients)
Watch Patient Journeys
Visit Our Centre
Are You the Right Candidate for EYE Care
Fill the form & we will tell you if Eye care treatment is right for you. Its Free!
Is It Rare?
The short answer is… it depends on what you mean by “rare.”
Globally, keratoconus is classified as an uncommon but not extremely rare condition. Statistically speaking, it affects approximately 1 in 2,000 people. But this number can vary based on where you live, your age, and even your genetic background.
⇒Why Isn’t the Prevalence Clear-Cut?
There are a few reasons why the prevalence of keratoconus varies:
1. Improved Diagnostic Tools
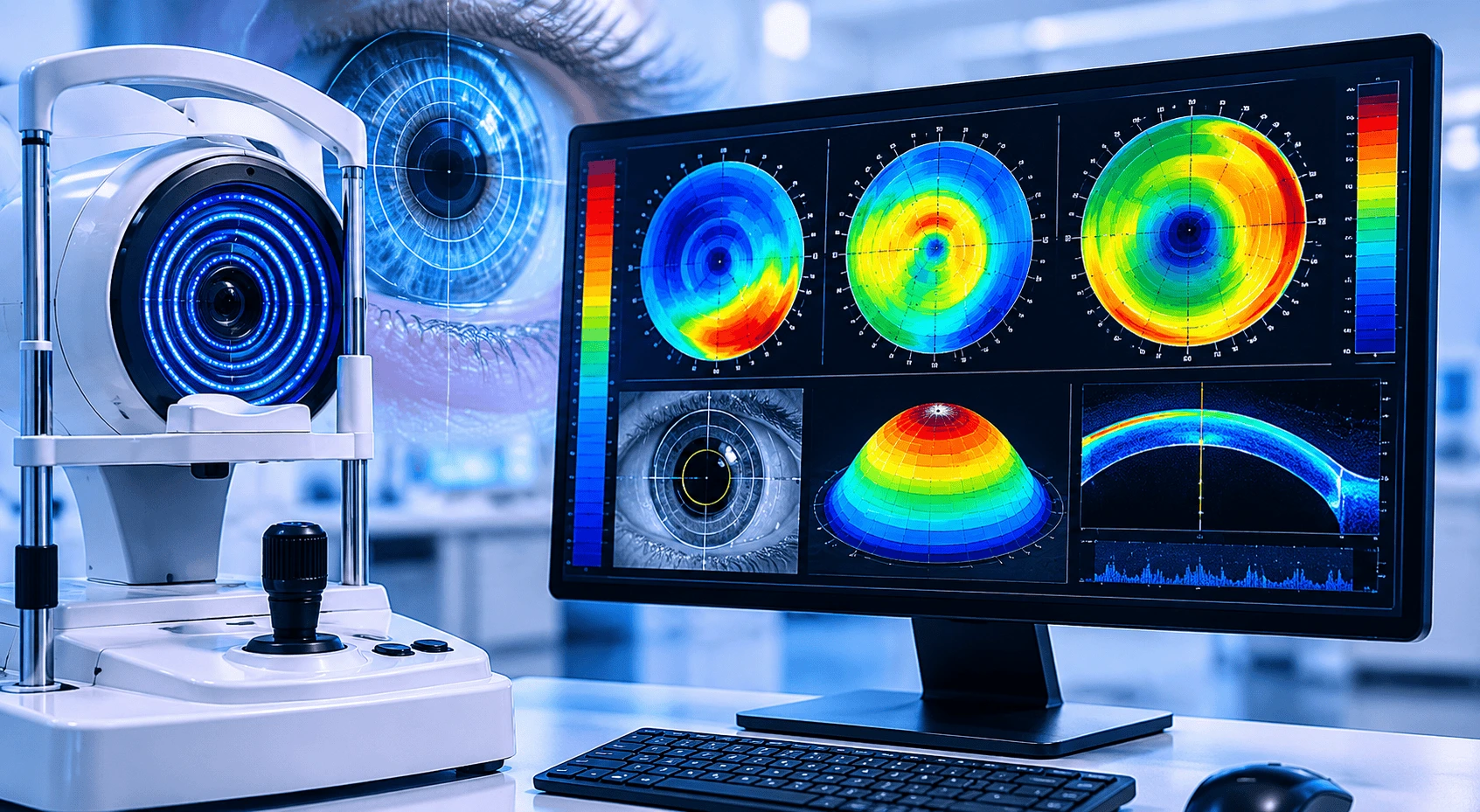
Thanks to advancements in eye care technology, we’re better at catching keratoconus early. For example, sophisticated equipment like topography (which maps your cornea’s shape) can detect mild cases that might’ve been missed in the past. This might make keratoconus look more common now than it did decades ago.
2. Differences Across Populations
Certain populations have a higher prevalence of keratoconus. One study found that it’s more common in parts of the Middle East, South Asia, and Central Asia compared to Europe and North America. For instance, research suggests countries like Saudi Arabia and India see keratoconus rates closer to 1 in 500 people.
3. Mild Cases Go Undiagnosed
Some people with very mild keratoconus might never experience noticeable symptoms. Because of this, they may never visit an eye doctor for a formal diagnosis, which keeps them out of the statistics.
⇒Is Keratoconus Rarer Than Other Eye Conditions?
Compared to something like nearsightedness or age-related macular degeneration, yes, keratoconus is much less common. But when you start comparing it to truly rare eye diseases, like retinoblastoma or aniridia, keratoconus is definitely less rare.
Who’s Most Likely to Develop Keratoconus?
Keratoconus isn’t entirely random. Certain factors may increase your risk, making it less “rare” in some groups than others:
- Age
Keratoconus often shows up in the teen years or early adulthood (between ages 10 and 25). It can get worse during these years, but progression typically slows down by your 30s or 40s.
- Genetics
Does keratoconus run in families? Yes, there’s evidence to suggest a genetic link. If someone in your family has it, your chances of developing it go up.
- Frequent Eye Rubbing
While this doesn’t “cause” keratoconus outright, excessive rubbing can weaken the cornea, possibly speeding up its progression.
- Underlying Conditions
Keratoconus is sometimes seen in people with certain conditions like Down syndrome, connective tissue disorders (like Marfan syndrome), or asthma, especially if there’s a lot of eye rubbing involved.
Does Geography Matter?
Absolutely. Keratoconus prevalence isn’t equal worldwide. Here are some fascinating geographic variations:
- Higher Prevalence Areas:
Countries like India, Iran, and Saudi Arabia report higher rates, likely due to genetic factors and environmental influences like sun exposure and dry weather.
- Lower Prevalence Areas:
Many European countries and the U.S. report prevalence rates closer to the global average (1 in 2,000). That said, these numbers might increase as diagnostics improve.
Why Does It Matter if Keratoconus Is Rare?
You might be thinking, “Okay, so keratoconus isn’t super common, but what does that really mean for me?” Here’s the thing:
- Early Diagnosis Is Key
Because it’s less common than near- or farsightedness, keratoconus can sometimes go unnoticed until it progresses.
That’s why being aware of the condition is so important. If you notice blurry vision, ghosting, or sensitivity to light that doesn’t improve with glasses, it’s worth seeing a specialist.
- Specialized Care Is Essential
Unlike widespread vision problems, keratoconus requires treatments that aren’t typically part of standard optometry care.
From custom contact lenses to groundbreaking procedures like corneal cross-linking, the earlier you’re diagnosed, the more options you’ll have.
- It’s Manageable
Even though it’s less common, advancements in eye care mean it’s highly manageable.
People with keratoconus today have access to treatments that can stabilize and even improve their vision, ensuring they lead full, active lives.
How You Can Take Action?
Whether you have keratoconus, suspect you might, or you’re reading up on it for a loved one, the most important thing is to act. Here are some actionable steps:
1. Watch for Symptoms
Symptoms like blurry vision, difficulty with night driving, or double vision warrant attention. If glasses or contacts don’t help, get checked out.
2. Find a Specialist
Not all eye doctors are equipped to diagnose and treat keratoconus. Look for someone who specializes in corneal disorders.
3. Explore Treatment
Treatments like corneal cross-linking can slow progression, and custom lenses can dramatically improve vision. Knowledge is power, and knowing your options makes all the difference.
4. Educate Yourself
Understanding keratoconus helps you feel empowered. From learning about the latest treatments to finding communities of people who share your experience, knowledge is your best ally.
Don’t Wait to Take Control
While keratoconus might be considered “uncommon,” the tools to diagnose and treat it are more accessible than ever.
If you’re experiencing symptoms, or if you’re just curious about this topic, don’t hesitate to reach out to an eye care professional.
Schedule an appointment today, and take proactive steps toward protecting and preserving your vision.
Remember, you’re not alone in this, and with the right care, there’s a bright, clear future ahead.
Wavelight Plus Corneal Mapping: How 100,000 Elevation Points Transform Vision Correction
Discover how Wavelight Plus corneal mapping uses 100,000 el…
Why is Wavelight Plus the Best Treatment for Patients with Irregular Astigmatism?
Discover why Wavelight Plus is ideal for irregular astigmati…
Why Wavelight Plus is Called “Topography-Guided” and Why It Matters for Night Vision?
Wavelight Plus is referred to as “topography-guided” because…