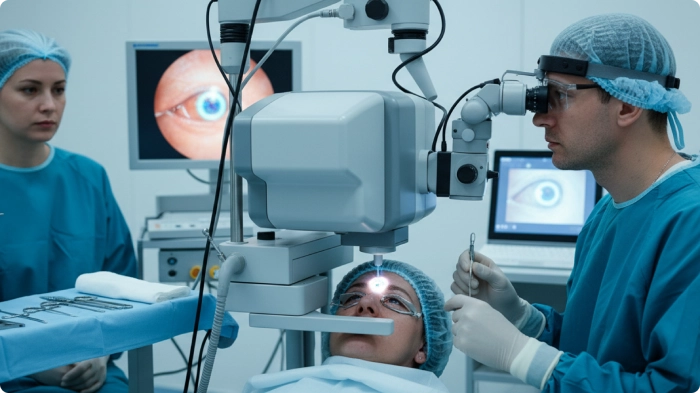
What to Do After a Failed SMILE Eye Procedure?
If you believe your SMILE eye procedure has failed (persistent blurry vision, intense halos, or pain), you must act immediately to manage the situation and, if necessary, arrange for an enhancement.
Medically Reviewed By:
Dr Advaith Sai Alampur
Leading LASIK & Refractive Surgery Expert
Condition:
Myopia
(Near sightedness)
Treatment:
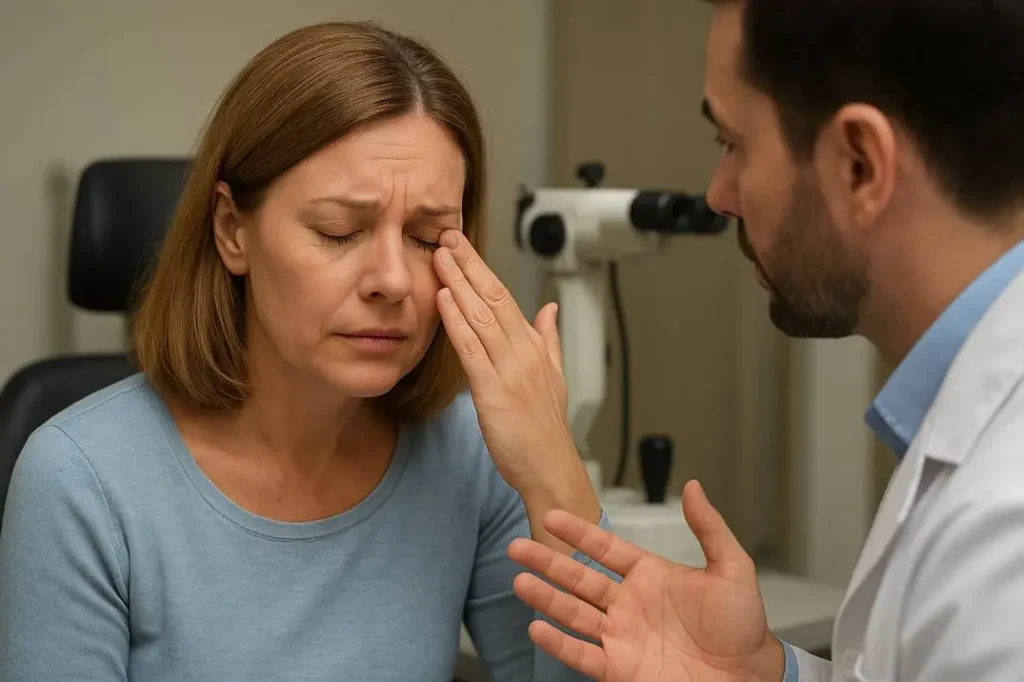
If you’re worried that your SMILE eye procedure didn’t go as planned, you’re not alone—and you’re not stuck.
Most issues after SMILE can be corrected or managed, and the earlier we evaluate your eyes, the better your outcome is likely to be.
In this guide, I’ll walk you through what “failed” can mean, the immediate steps to take, how we diagnose the problem, the treatment options available (from simple drops to enhancement surgery), how to cope emotionally, and how to reduce the chance of future issues.
My goal is to help you feel informed, safe, and clear about what comes next.
In this article
- LASIK reshapes the cornea to correct nearsightedness, farsightedness, and astigmatism.
- The procedure is FDA-approved, safe, and uses modern laser technology for precision.
- Candidates should be over 18, have a stable prescription, and healthy corneas.
- Short-term side effects can include dry eyes, halos, glare, or temporary vision fluctuations.
- Most patients achieve stable, long-term vision improvement and are satisfied with results.
- LASIK doesn’t stop natural age-related changes, so reading glasses may still be needed later.




(Put Real times images and shorts of Dr Avdaith Sai Consulting, Operating on Patients)
Watch Patient Journeys
Visit Our Centre
Small Incision Lenticule Extraction (SMILE) is a laser vision correction procedure that reshapes the cornea through a tiny incision.
It’s well-established, with high satisfaction and safety in suitable candidates. Still, no procedure is risk-free. When patients say “failed,” they usually mean one of the following:
- Undercorrection or overcorrection: Your vision didn’t reach the expected target (for example, still needing glasses for distance).
- Residual refractive error: Blurry vision, ghosting, or halos especially at night.
- Dry eye symptoms: Grittiness, fluctuating vision, or light sensitivity.
- Visual quality concerns: Halos, glare, starbursts, or reduced contrast.
- Interface issues: Debris or inflammation at the corneal interface.
- Epithelial ingrowth (rare after SMILE): Surface cells migrating under the corneal flap-equivalent plane.
- Irregular astigmatism: Distorted or fluctuating vision due to uneven corneal shape.
- Infection or inflammation: Pain, redness, sharp decline in vision—this needs urgent attention.
- Ectasia (rare): Progressive thinning and bulging of the cornea causing worsening vision.
Most of these are not permanent failures. Many improve with time or respond to targeted treatments. True “failure” is uncommon, and even then, we usually have pathways to restore good functional vision.
Are You the Right Candidate for Smile pro?
Fill the form & we will tell you if Smile pro is right for you. Its Free!
Immediate steps to take if you think your SMILE failed
1) Don’t wait—contact your clinic
If you’re noticing significant pain, sudden blur, increasing redness, light sensitivity, or a rapid decline in vision, call your surgeon’s office today. Early review can rule out infection or inflammation that needs prompt treatment.
2) Use your prescribed drops exactly as directed
Continue any antibiotic, steroid, and lubricating drops unless your surgeon advises changes. If you’ve run out of drops or stopped them early, let your clinician know.
3) Avoid eye rubbing and water exposure
Rubbing increases irritation and can disturb corneal healing. Avoid swimming and hot tubs. In the shower, keep your eyes closed and pat dry.
4) Protect your eyes
Use sunglasses outdoors to reduce glare and light sensitivity. At night, a shield can help you avoid accidental rubbing during sleep.
5) Gather a symptom diary
Note when your vision is better or worse (morning vs evening), what symptoms you feel (dryness, ghosting, halos), and how long they’ve been present. This helps your surgeon tailor treatment.
A proper evaluation gives us a clear map of what’s going on. Expect some or all of the following:
- Visual acuity and refraction: Checks how well you see and your prescription. We compare this to your pre-op numbers.
- Corneal topography and tomography: Detailed maps of corneal shape and thickness to detect irregular astigmatism or early ectasia.
- Tear film tests: To assess dry eye and meibomian gland function.
- Slit-lamp exam: Looks for interface haze, debris, inflammation, or epithelial ingrowth.
- Pupil size assessment: Large pupils can aggravate night glare and halos.
- Optical coherence tomography (OCT): High-resolution imaging of corneal layers and the interface.
- Wavefront aberrometry: Measures higher-order aberrations that can cause glare and starbursts.
This assessment helps us decide whether time, drops, lid therapy, or an enhancement will solve the problem.
Common post-SMILE problems and how we manage them?
Enhancement isn’t a failure—it’s a fine-tuning step used across laser vision procedures. Timing and method depend on corneal health and stability.
1.Timing
We usually wait until your refraction is stable on at least two visits, often 3–6 months after SMILE. If there’s a clear, correctable issue like interface debris, we act sooner.
2.Options
⇒PRK enhancement:
Pros: Preserves corneal strength by treating on the surface; excellent for small corrections and irregularities.
Cons: Longer recovery, some discomfort for a few days, temporary haze risk (managed with drops and, in select cases, mitomycin-C).
3.LASIK conversion:
Pros: Faster visual recovery and comfort, good for certain corrections.
Cons: Requires creating or converting to a flap; slightly higher dry-eye risk than PRK; suitability depends on corneal thickness and shape.
4.Repeat SMILE:
Less common; may be considered in select scenarios depending on your anatomy and the laser platform.
5.Phakic IOL (ICL) or lens-based options:
For larger residual errors or when corneal tissue is limited, implantable lenses can deliver excellent quality without additional corneal reshaping.
Your surgeon will calculate the safest route based on your corneal thickness, topography, and visual goals.
1.Call your surgeon’s office and book the earliest assessment.
2.Use prescribed drops as directed; don’t stop steroids abruptly unless advised.
3.Increase preservative-free lubrication.
4.Avoid contact lenses unless your surgeon recommends them for comfort (for example, a bandage lens).
5.Rest your eyes: frequent breaks from screens and good hydration.
6.Note red flags: increasing pain, sudden vision loss, pus-like discharge—seek urgent care the same day.
1.Week 1–4: Dryness and fluctuation are common. Lubrication and time often help.
2.Month 1–3: Most people stabilise; if you have lingering blur, we reassess tear film, residual prescription, and corneal maps.
3.Month 3–6: If your vision is not where we want it but is stable and the cornea is healthy, we plan enhancement.
4.Beyond 6 months: We can still enhance if indicated. Very late issues like ectasia are rare but treatable if identified early.
It’s normal to feel disappointed or worried after vision surgery, especially if your expectations were high. Here’s how to cope while we sort things out:
1.Get clear information: Ask for your diagnosis, likely timeline, and plan A/plan B. Knowing the path reduces fear.
2.Focus on the “controllables”: Use your drops, keep appointments, protect your eyes, and follow the plan.
3.Temporary aids are not defeat: A brief return to glasses or contact lenses is a bridge, not the destination.
4.Seek support: Talk with someone who understands—family, a friend, or a support group. If anxiety is affecting sleep or work, consider speaking with your GP or a counsellor.
5.Celebrate small wins: Less glare this week? More comfortable screen time? These are signs you’re moving in the right direction.
1.Choose the right time for enhancement
Wait for stability. Enhancing too early risks chasing a moving target.
2.Optimise the ocular surface
Treat dry eye before any enhancement: warm compresses, lid hygiene, omega-3s (if appropriate), lubricants, and sometimes prescription anti-inflammatories.
Screen habits: Follow the 20-20-20 rule and increase ambient humidity.
3.Thorough pre-enhancement screening
Updated corneal topography/tomography and pachymetry.
Wavefront measurements for quality-of-vision concerns.
Ensure adequate residual stromal bed and safe tissue calculations.
Rule out early ectasia or keratoconus patterns.
4.Surgeon and centre selection
Look for surgeons who perform a high volume of SMILE and enhancements.
Ask about their enhancement rates and protocols, and whether they offer PRK, LASIK conversion, cross-linking, and phakic IOLs.
Confirm access to modern diagnostics (scheimpflug tomography, epithelial mapping, aberrometry).
5.Lifestyle factors
Avoid eye rubbing—especially during allergy season. Treat allergies promptly.
Wear UV-blocking sunglasses outdoors.
Keep systemic conditions (like diabetes) well controlled, as they can affect healing.
1.Did my SMILE definitely fail?
Not necessarily. Early fluctuations, dryness, or mild blur are common and often improve. A “failed” result usually means persistent issues beyond the early healing window. Let’s assess before labelling it a failure.
2.Will I need another surgery?
Maybe. Many patients improve with time, drops, and tear film treatment alone. If a stable prescription remains, a minor enhancement often brings you to the goal.
3.Is an enhancement riskier?
Enhancements carry risks, but when planned carefully with stable measurements and a healthy cornea, they’re usually safe and effective. We choose the method with the best safety margin for your eyes.
4.Can glasses or contacts help in the meantime?
Yes. A temporary pair of glasses or soft contact lenses can make day-to-day life easier while we monitor your healing or plan an enhancement.
5.Could I have ectasia?
It’s rare after SMILE, especially if pre-op screening was thorough. If we’re concerned, we use tomography to check. If present, cross-linking can stabilise the cornea.
6.How long until I can drive at night comfortably again?
For many, night symptoms improve over 1–3 months as the tear film stabilises. If residual prescription or aberrations persist, enhancement can help.
- Today: Call your clinic, describe your symptoms, and book the earliest appointment.
- This week: Increase preservative-free lubrication, avoid rubbing, protect eyes from glare, and keep a symptom diary.
- At your visit: Ask for updated refraction, topography/tomography, tear film assessment, and a clear plan.
- Next 4–8 weeks: Follow treatment (drops, lid care, plugs if recommended). Reassess. If vision stabilises but isn’t ideal, discuss enhancement options.
- Beyond 3 months: If stable and safe, consider PRK or LASIK conversion enhancement; if not safe, discuss alternatives like phakic IOLs or specialty contacts.
A disappointing outcome after SMILE is stressful, but it’s rarely the end of the story.
Most issues have clear solutions—some simple, some more involved—and with careful diagnosis and a tailored plan, we can usually restore comfortable, sharp vision.
Reach out for an appointment, bring your questions, and we’ll map the next steps together.
LASIK for Pilots in India: A Guide to Vision Standards & Safety
LASIK for pilots in India: DGCA rules, Armed Forces standard…
AI in LASIK Surgery: How Artificial Intelligence Is Transforming Vision Correction (2026)
SMILE Pro preserves 80% more corneal nerves than LASIK by us…
Environmental Factors and LASIK Outcomes: How Pollution and UV Exposure Influence Success and Longevity
Learn how pollution and UV exposure affect LASIK outcomes, h…